Researchers have identified a vital epitope on the CD95 receptor, which can trigger programmed cell death and may enhance cancer treatments. The findings could be crucial for future therapeutic strategies.
A group of researchers from the UC Davis Comprehensive Cancer Center identified a crucial epitope (a protein section that can activate the larger protein) on the CD95 receptor that can cause cells to die. This new ability to trigger programmed cell death could open the door for improved cancer treatments. The findings were recently published in the journal Cell Death & Differentiation.
Also referred to as Fas, the CD95 receptors are often termed “death receptors”. These protein structures are found inside cell membranes and, upon activation, release a signal that causes the cells to self-destruct.
Modulating Fas may also extend the benefits of chimeric antigen receptor (CAR) T-cell therapy to solid tumors like ovarian cancer.
“We have found the most critical epitope for cytotoxic Fas signaling, as well as CAR T-cell bystander anti-tumor function,” said Jogender Tushir-Singh, an associate professor in the Department of Medical Microbiology and Immunology and senior author of the study.
“Previous efforts to target this receptor have been unsuccessful. But now that we’ve identified this epitope, there could be a therapeutic path forward to target Fas in tumors,” Tushir-Singh said.
Finding better cancer therapies
Cancer is generally managed with surgery, chemotherapy, and radiotherapy. These treatments may work initially, but in some cases, therapy-resistant cancers often return. Immunotherapies, such as CAR T-cell-based immune therapies and immune checkpoint receptor molecule activating antibodies, have shown tremendous promise to break this cycle. But they only help an extremely small number of patients, especially in solid tumors such as ovarian, triple-negative breast cancer, lung, and pancreas.
T cells are a type of immune cells. CAR T-cell therapies involve engineering patient T cells by grafting them with a specific tumor-targeting antibody to attack tumors. These engineered T cells have shown efficacy in leukemia and other blood cancers but have failed repeatedly to provide success against solid tumors. The reason is that tumor microenvironments are good at keeping T cells and other immune cells at bay.
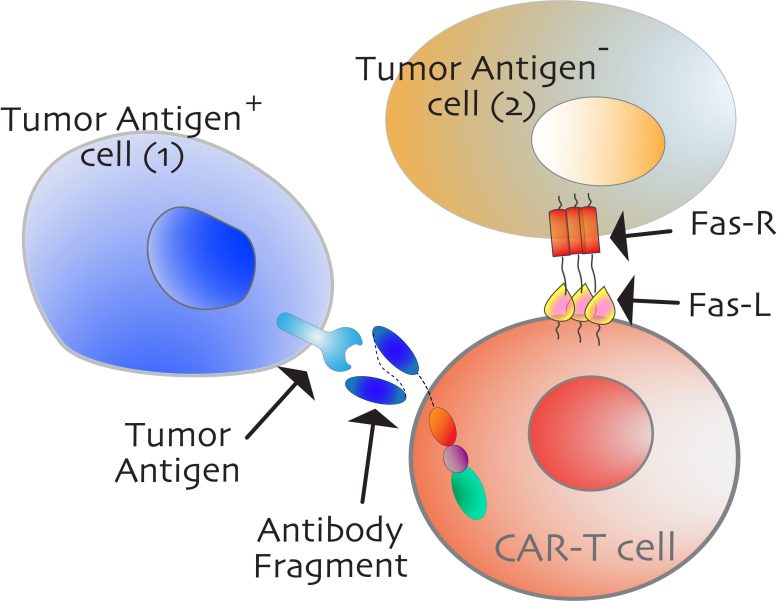
Antigen-positive tumor cell (blue, left) is a direct target of CAR T-cells (light red) due to high-affinity antibody-antigen contacts. On the contrary, an antigen-negative tumor cell (light golden, right) is killed by Fas-mediated “bystander” killing. Cancer patients with high Fas-expression are expected to respond significantly better to immunotherapies. Credit: UC Davis
“These are often called cold tumors because immune cells simply cannot penetrate the microenvironments to provide a therapeutic effect,” said Tushir-Singh. “It doesn’t matter how well we engineer the immune receptor activating antibodies and T cells if they cannot get close to the tumor cells. Hence, we need to create spaces so T cells can infiltrate.”
Death receptors do precisely what their name implies — when targeted, they trigger programmed cell death of tumor cells. They offer a potential workaround that could simultaneously kill tumor cells and pave the way for more effective immunotherapies and CAR T-cell therapy.
Developing drugs that boost death receptor activity could provide an important weapon against tumors. However, though drug companies have had some success targeting the Death Receptor-5, no Fas agonists have made it into clinical trials. These findings could potentially change that.
The right target
While Fas plays an essential role in regulating immune cells, Tushir-Singh and his colleagues knew they might be able to target cancer cells selectively if they found the right epitope. Having identified this specific epitope, he and other researchers can now design a new class of antibodies to selectively bind to and activate Fas to potentially destroy tumor cells specifically.
Other research in animal models and human clinical trials has shown that Fas signaling is fundamental to CAR T success, particularly in tumors that are genetically heterogeneous. Genetically heterogeneous tumors have a mix of different cell types, which can respond differently to treatment.
A Fas agonist could generate a CAR-T bystander effect, in which the treatment destroys cancer cells that lack the molecule the tumor-targeting antibody is designed to hit. In other words, activating Fas may destroy cancer cells and improve CAR T efficacy, a potential one-two punch against tumors.
In fact, the study showed tumors with a mutated version of the epitope of Fas receptors will not respond to CAR T at all. This finding could lead to new tests to identify which patients will benefit most from CAR T-cell immunotherapy.
“We should know a patient’s Fas status — particularly the mutations around the discovered epitope — before even considering giving them CAR T,” Tushir-Singh said. “This is a definitive marker for bystander treatment efficacy of CAR T therapy. But most importantly, this sets the stage to develop antibodies that activate Fas, selectively kill tumor cells, and potentially support CAR T-cell therapy in solid tumors.”
Reference: “Characterizing the regulatory Fas (CD95) epitope critical for agonist antibody targeting and CAR-T bystander function in ovarian cancer” by Tanmoy Mondal, Himanshu Gaur, Brice E. N. Wamba, Abby Grace Michalak, Camryn Stout, Matthew R. Watson, Sophia L. Aleixo, Arjun Singh, Salvatore Condello, Roland Faller, Gary Scott Leiserowitz, Sanchita Bhatnagar and Jogender Tushir-Singh, 14 October 2023, Cell Death & Differentiation.
DOI: 10.1038/s41418-023-01229-7
Additional authors include Tanmoy Mondal, Himanshu Gaur, Brice E. N. Wamba, Abby Grace Michalak, Camryn Stout, Matthew R. Watson, Sophia L. Aleixo, Arjun Singh, Roland Faller, Gary Scott Leiserowitz and Sanchita Bhatnagar from UC Davis. and Salvatore Condello from Indiana University School of Medicine.
The study was funded by the National Cancer Institute and the U.S. Department of Defense.

Sarah Carter is a health and wellness expert residing in the UK. With a background in healthcare, she offers evidence-based advice on fitness, nutrition, and mental well-being, promoting healthier living for readers.